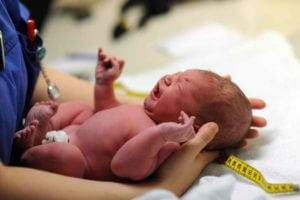
Postpartum flow is as much a part of pregnancy as conception and birth. It begins shortly after delivery and lasts an average of four weeks.
During this time, it changes in terms of quantity, color and composition. If the discharge suddenly decreases or develops an unpleasant odor, you should be careful. – because then it could be a consequential postpartum congestion caused by a bagel or similar. Influences. Here you can find out how it occurs, what causes it and why it can be dangerous.
Table of contents
Postpartum Flow As A Biological Task
Your body is a miracle: for nine months it does everything to promote the development of your baby. But as soon as the little one is born, it vehemently fights against the pregnancy. With contractions and postpartum flow, it tries to eliminate the last traces of the big event in the uterus.
The reasons for this are manifold and could not be more different: On the one hand, your organism wants to recover from “babysitting”, because taking care of two people in a very small space is hard work for it. At the same time, it struggles to restore the “normal state”; that is, to prepare everything for another pregnancy.
- Also interesting:
- The best pacifiers
- Recommended diaper bags
- The best breast pumps
With this ambiguous task, he follows a millennia-old plan. To enable and promote reproduction is one of its basic concerns. It comes right after breathing, eating, and sleeping, and ranks far ahead of culture, education, and other civilian bells and whistles.
It’s understandable that your body doesn’t want to be delayed unnecessarily. Because it takes different lengths of time after each delivery before pregnancy is possible again, it gets to work immediately. It takes a series of drastic measures to “clean” the uterus.
Like a rolling squad, he eliminates anything that reminds him of the little lodger of the last few months. This sounds as insensitive as it is – and can be particularly upsetting after a miscarriage.
But the onset of postpartum flow is necessary to protect your body from disease. If residue remains in the uterus or coils form, germs can colonize and lead to what is known as puerperal fever or postpartum fever.
Postpartum Congestion As A Cause Of Puerperal Fever
In earlier times, this condition was very common and cost the lives of many new mothers. Today, it occurs much less frequently; however, it is still present because the circumstances that lead to puerperal fever have not changed.
It affects women who become infected with bacteria during or after childbirth. These do not have to be specific pathogens – but simply germs that harm your body. In addition to the cholera-causing Escherichia coli and the gonorrhea-causing Neisseria gonorrhoeae, various anaerobes or streptococci lead to puerperal fever.
These germs find many transmission routes; they are virtually everywhere and cannot be excluded in principle. However, for them to become “active”, certain general conditions must prevail. The pathogens need a “breeding ground” and an environment free of disturbances.
They find both in wound fluids or accumulations of secretions such as postpartum congestion. It occurs when your body does not continue to work as planned after birth – for example, because it is prevented from doing so by external circumstances.
Postpartum Flow Is A Completely Natural Process
The most effective measure against postpartum congestion and the resulting fever is a natural birth. While it creates the “best” conditions for invading germs; it also brings about a series of “self-cleansing” measures that lasts a fraction as long as pregnancy – around eight weeks.
After delivery, your lower body has a direct “wire” to the outside world. In the course of childbirth, the cervix has stretched and now forms a wide-open corridor between the vagina and the uterus. Germs have an easy time here. They can penetrate unhindered to the “innermost core”, seek out optimal living conditions and promote coagulum or puerperal fever.
Usually, the female organism counteracts this: 10-20 minutes after your baby is born, there are renewed contractions, the so-called afterpains. They cause the placenta to detach from the uterine wall and transport everything that is no longer needed outside.
The midwife can help this process along with certain hand movements; above all, however, she must check whether the afterbirth is complete, because residues remaining in the uterus are the main cause of discomfort in the postpartum period.
However, your body also counteracts this eventuality on its own: In addition to the afterbirth, it secretes 250-500 ml of blood – a kind of wiping water for the now empty uterus. It comes from the wound left by the detached placenta on the cavity wall and flushes away the pathogens of puerperal fever with the afterbirth.
If some of them are particularly persistent, they find a great place to stay in the placenta wound area. But they can’t just settle in, because your body takes countermeasures. Over several weeks, the dilated uterus contracts bit by bit.
This produces the so-called postpartum flow – a mixture of blood, secretions and tissue fragments. It also helps to transport any puerperal germs that may have entered to the outside and to prevent the development of coagulum.
Factors That Can Disrupt Postpartum Flow
Sometimes, however, the mixture does not drain properly and accumulates in the uterus. Such lochia can occur under the following conditions:
- After a cesarean section
- If the cervix is stuck together
- Due to residual tissue
- Due to clotted blood (coagulum)
- In case of insufficient contractions
Find out about the occurrence, duration and appearance of lochia even before the birth. Monitoring its proper “flow” is one of the preventive measures against puerperal fever.
As soon as there is a noticeable change in the amount, color, smell or consistency, you should become alert. A midwife or doctor can tell you if they have detected coagulum and your suspicion of puerperal congestion is well-founded.
Postpartum Flow As A Long Regeneration Phase
There is no general answer to this question, because the discharge after childbirth does not follow a rule. It depends, among other things, on how the delivery proceeds and how long it lasts, whether the pregnancy was terminated prematurely or whether your baby was born by Caesarean section.
All of these factors can have a positive or negative effect on lochia. For example, naturally born children are still the best guarantee for the continuous discharge of wound fluid, blood and tissue remnants – and thus the most effective means in the fight against coagulum and invading or invaded germs.
Whether or not you are breastfeeding also has an effect on the flow and how long it lasts – because every time your baby lays on your breast or sucks, your body releases oxytocin.
This hormone promotes the contraction of the uterus and thus naturally counteracts the flow congestion. The muscle contractions help to expel fluid and tissue more quickly and effectively than mothers who (have to) bottle-feed their babies.
However, breastfeeding does not necessarily protect you from postpartum congestion. There are many reasons why the natural process can stall or become a breeding ground for bacteria. Accidental infections with germs that cause puerperal fever are only one of them.
Much more frequently, a disturbance can be traced back to quite mundane reasons, whereby diseases in the puerperium catch up with their historical predecessors. Then as now, puerperal congestion and the resulting puerperal fever can be caused by improper hygiene.
Recommendations For Postpartum Care
If you have read carefully, you will have noticed that we are not writing about a lack of care – but in fact also mean excessive cleanliness. Discharge after delivery has a natural cause: the birth of your child.
It comes from your “deepest inside” and is composed of organic substances. There is nothing disgusting, wrong or unhealthy about it per se and therefore there is no reason to treat postpartum flow like leprosy.
Consider its scheduled discharge a gift from nature, which knows best what is good for your body. It regulates the amount and the discharge of the fluid-tissue mixture all by itself as long as you let it and no obstacles are put in its way.
If you make sure that the flow can leave the vagina unhindered and is collected by a suitable pad, you are instinctively doing the right thing. Tampons are not suitable for this situation.
On the one hand, because they only absorb fluid, but retain tissue – and thus promote the formation of coagulum and postpartum congestion. Secondly, because they irritate the already strained vagina – no matter how smoothy, silky or softy they are made.
And finally, every foreign body that you insert is a potential germ litter. Under “normal” circumstances, using tampons is not a problem; however, during lochia there is increased sensitivity.
The same is true for sex during the postpartum or puerperal period. Don’t misunderstand each other: Your partner’s body parts are of course not taboo – but they considerably increase the risk of contracting puerperal fever.
However, it would be wrong to overdo any hygiene. You do not need disinfectants or similar preparations to protect yourself from puerperal congestion. Normal body care with clean water or pH-neutral soap is sufficient.
If the maternity hospital has bidets, this is ideal, because they support cleaning and can have a soothing effect on your genital tract. However, a jug of warm water will serve the same purpose.
In addition, you should use absorbent, breathable pads and disposable briefs, which you should change regularly, checking the consistency of your postpartum flow.
As soon as the flow decreases, you can use private underwear and commercially available pads with higher absorbency. However, here too, make sure you use natural materials and change them appropriately. You should avoid synthetic fibers, perfumed or dyed pads and lying down for too long, as they promote moisture and heat buildup – which in turn affects the flow of your period.
Last but not least, your diet also has an influence on the natural process in your body. As it releases fluids, it needs replenishment in the form of non-alcoholic, low-sugar drinks such as unsweetened tea, natural juice or water.
The ingredients in fruits and vegetables provide it with much of what it needs to regenerate. By keeping the flow of fluids “going”, you also prevent coagulation and postpartum congestion. It’s that simple and effective.
Postpartum As A Time-out: What You Need To Know About It
But don’t get the impression that postpartum problems are caused by your behavior alone. There are numerous other reasons why “the course of events” gets stuck and promotes postpartum congestion.
Originally, it served to spare the new mother and to allow her time with the child. For this purpose, she was released from all obligations. She did not have to do housework or field work, was exempt from going to church, and could not be prosecuted. Instead of her, neighbors, friends and midwives took care of everything.
Unpleasant sensations and the stress caused by excessive or overwhelming attendance can lead to the onset of postpartum congestion. Midwives know the problem and try to point it out to mothers and their families.
In extreme cases, they relieve the blockage with an emotional stimulus. As soon as the tears that have been so laboriously held back are allowed to flow, the postpartum flow also “gets going” again. In the case of physical causes, it is not quite so easy to let the dam burst and release lochia.
But fortunately, factors that come into question are now well known – and can be monitored accordingly. One of the most common causes of coeliac formation and resulting lochia is an excessively tilted uterus.
Whether it is “tilted” backward or forward, it interferes with the flow of the lochia and thus can contribute to the engorgement. Furthermore, the stomach, intestines and bladder can interfere with the flow of the lochia.
If they are full, they press on other internal organs and can cause discomfort. To prevent congestion and coagulation, a postpartum diet should include several small, easily digested meals – the residue of which you must “release” by going to the toilet regularly.